Otitis externa
| Otitis externa | |
|---|---|
| Classification and external resources | |
A severe case of otitis externa. Note the narrowing of the external auditory channel and swelling of the auricle. |
|
| ICD-10 | H60. |
| ICD-9 | 380.1-380.2 |
| DiseasesDB | 9401 |
| MedlinePlus | 000622 |
| eMedicine | ped/1688 emerg/350 |
| MeSH | D010032 |
Otitis externa (also known as "External otitis"[1] and "Swimmer's ear"[1]) is an inflammation of the outer ear and ear canal. Along with otitis media, external otitis is one of the two human conditions commonly called "earache". It also occurs in many other species. Inflammation of the skin of the ear canal is the essence of this disorder. The inflammation can be secondary to dermatitis (eczema) only, with no microbial infection, or it can be caused by active bacterial or fungal infection. In either case, but more often with infection, the ear canal skin swells and may become painful and/or tender to touch.
Contents |
Classification
In contrast to the chronic otitis externa, acute otitis externa is predominantly a microbial infection, occurs rather suddenly, rapidly worsens, and becomes very painful and alarming. The ear canal has an abundant nerve supply, so the pain is often severe enough to interfere with sleep. Wax in the ear can combine with the swelling of the canal skin and any associated pus to block the canal and dampen hearing to varying degrees, creating a temporary conductive hearing loss. In more severe or untreated cases, the infection can spread to the soft tissues of the face that surround the adjacent parotid gland and the jaw joint, making chewing painful. In its mildest forms, external otitis is so common that some ear nose and throat physicians have suggested that most people will have at least a brief episode at some point in life. While a small percentage of people seem to have an innate tendency toward chronic external otitis, most people can avoid external otitis altogether once they understand the intricate mechanisms of the disease.
The skin of the bony ear canal is unique, in that it is not movable but is closely attached to the bone, and it is almost paper thin. For these reasons it is easily abraded or torn by even minimal physical force. Inflammation of the ear canal skin typically begins with a physical insult, most often from injury caused by attempts at self-cleaning or scratching with cotton swabs, pen caps, finger nails, hair pins, keys, or other small implements. Another causative factor for acute infection is prolonged water exposure in the forms of swimming or exposure to extreme humidity, which can compromise the protective barrier function of the canal skin, allowing bacteria to flourish; hence the name, "swimmer's ear". Densely impacted wax, usually caused by enthusiastic use of cotton swabs, can put enough pressure on the ear canal skin to injure it and initiate infection. A sensation of blockage or itching can prompt attempts to clean, scratch, or open the ear canal, which potentially worsens and perpetuates the condition. The cotton fibers of a swab are abrasive to the thin, fixed canal skin. Self-manipulative measures to improve the condition often make it worse and are to be discouraged, since it is a blind exercise that can result in significant injury to the ear. Production of wax by glands in the canal may be hindered by external otitis. The exact function(s) of earwax (cerumen) is a subject that is open to speculation, since there is very little research regarding its function. Some caretakers feel strongly that earwax has a protective function with respect to infection and that a little earwax in the ear canal is a good thing. A natural question would be how one may be able to clean their own ears; it is well established that in most people the top layer of the ear canal skin normally migrates toward the ear opening, essentially sweeping the canal on a continuing basis. In other words, a normal ear canal is self-cleaning. This self-cleaning physiologic feature fails in some patients, especially in late life, and periodic cleaning by a physician can be necessary. The most controlled and least painful means of cleaning impacted wax or dead skin from the ear canal is by using a binocular surgical microscope, which frees the examiner's hands to instrument the ear and provides the magnification and depth perception needed to avoid traumatizing the delicate canal skin and eardrum.
Symptoms
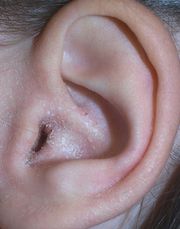
Pain is the predominant complaint and the only symptom directly related to the severity of acute external otitis. Unlike other forms of ear infections, the pain of acute external otitis is worsened when the outer ear is touched or pulled gently. Pushing the tragus, the tablike portion of the auricle that projects out just in front of the ear canal opening, so typically causes pain in this condition as to be diagnostic of external otitis on physical examination. Patients may also experience ear discharge and itchiness. When enough swelling and discharge in the ear canal is present to block the opening, external otitis may cause temporary conductive hearing loss.
Due to the fact that the ear and throat are often interconnected, irritation (whether it be in inflammation or a scratching sensation) is normal. However, excessive throat symptoms may likely point to the throat as the cause of the pain in the ear rather than the other way around.
Because the symptoms of external otitis lead many people to attempt to clean out the ear canal (or scratch it) with slim implements, self-cleaning attempts generally lead to additional trauma of the injured skin, so rapid worsening of the condition often occurs.
Causes, incidence, and risk factors
Swimming in polluted water is a common way to contract swimmer's ear, but it is also possible to contract swimmer's ear from water trapped in the ear canal after a shower, especially in a humid climate.[2] Constriction of the ear canal from bone growth (Surfer's ear) can trap debris leading to infection.[3] Saturation divers have reported Otitis externa during occupational exposure.[4][5][6] Even without exposure to water, the use of objects such as cotton swabs or other small objects to clear the ear canal is enough to cause breaks in the skin, and allow the condition to develop.[7] Once the skin of the ear canal is inflamed, external otitis can be drastically enhanced by either scratching the ear canal with an object, or by allowing water to remain in the ear canal for any prolonged length of time.
The two factors that are required for external otitis to develop are (1) the presence of germs that can infect the skin and (2) impairments in the integrity of the skin of the ear canal that allow infection to occur. If the skin is healthy and uninjured, only exposure to a high concentration of pathogens, such as submersion in a pond contaminated by sewage, is likely to set off an episode. However, if there are chronic skin conditions that affect the ear canal skin, such as atopic dermatitis, seborrheic dermatitis, psoriasis or abnormalities of keratin production, or if there has been a break in the skin from trauma, even the normal bacteria found in the ear canal may cause infection and full-blown symptoms of external otitis.[8]
Fungal ear canal infections, also known as otomycosis, range from inconsequential to very severe. Fungus can be saprophytic, in which there are no symptoms and the fungus simply co-exists in the ear canal in a harmless parasitic relationship with the host, in which case the only physical finding is presence of the fungus. If for any reason the fungus begins active reproduction, the ear canal can fill with dense fungal debris, causing pressure and ever-increasing pain that is unrelenting until the fungus is removed from the canal and anti-fungal medication is used. Most antibacterial ear drops also contain a steroid to hasten resolution of canal edema and pain. Unfortunately such drops make fungal infection worse. Prolonged use of them promotes growth of fungus in the ear canal. Antibacterial ear drops should be used a maximum of one week, but 5 days is usually enough. Otomycosis responds more than 95% of the time to a three day course of the same over-the-counter anti-fungal solutions used for athlete's foot.
The incidence of otitis externa is high. In the Netherlands, it has been estimated at 12–14 per 1000 population per year, and has been shown to affect more than 1% of a sample of the population in the United Kingdom over a 12 month period.[9]
Pathogens
The bacterial pathogens at the top of the list are Pseudomonas aeruginosa and Staphylococcus aureus, followed by a great number of other gram-positive and gram-negative species.[10] Candida albicans and Aspergillus species are the most common fungal pathogens responsible for the condition.
Diagnosis
When the physician looks in the ear, the canal appears red and swollen in well-developed cases of acute external otitis. The ear canal may also appear eczema-like, with scaly shedding of skin. Touching or moving the outer ear increases the pain, and this maneuvre on physical exam is very important in establishing the clinical diagnosis. It may be difficult for the physician to see the eardrum with an otoscope at the initial examination because of narrowing of the ear canal from inflammation and the presence of drainage and debris. Sometimes the diagnosis of external otitis is presumptive and return visits are required to fully examine the ear. Culture of the drainage may identify the bacteria or fungus causing infection, but is not part of the routine diagnostic evaluation. In severe cases of external otitis, there may be swelling of the lymph node(s) directly beneath the ear.
The diagnosis may be missed in early cases because the examination of the ear, with the exception of pain with manipulation, is normal or nearly normal. In some cases of early external otitis, the most striking visual finding in the ear canal is the lack of cerumen. As a moderate or severe case of external otitis resolves, weeks may be required before the ear canal again shows a normal amount of cerumen.
Prevention
The strategies for preventing acute external otitis are similar to those for treatment.
- Avoid inserting anything into the ear canal; use of cotton buds or swabs is the most common event leading to acute otitis externa.
- Most normal ear canals have a self-cleaning and self-drying mechanism, the latter by simple evaporation.
- After prolonged swimming, a person prone to external otitis can dry the ears using a small battery-powered ear dryer, available at many retailers, especially shops catering to watersports enthusiasts. Alternatively, drops containing dilute acetic acid (vinegar diluted 3:1) or Burow's solution may be used. It is especially important NOT to instrument ears when the skin is saturated with water, as it is very susceptible to injury, which can lead to external otitis.
- Avoid swimming in polluted water.
- Avoid washing hair or swimming if very mild symptoms of acute external otitis begin
- Although the use of earplugs when swimming and shampooing hair may help prevent external otitis, there are important details in the use of plugs. Hard and poorly fitting ear plugs can scratch the ear canal skin and set off an episode. When earplugs are used during an acute episode, either disposable plugs are recommended, or used plugs must be cleaned and dried properly to avoid contaminating the healing ear canal with infected discharge. One simple method of fabricating soft waterproof disposable ear plugs is with cotton balls and petroleum jelly. These jelly coated cotton balls are NOT inserted into the ear canal, but pressed into the auricle to cover the opening of the canal. Poorly fitted head sets can also bring on an episode caused by friction between the ear and phone muffs. It is important to wear small head phones that do not cover the whole ear.
Treatment
The goal of treatment is to cure the infection and to return the ear canal skin to a healthy condition. When external otitis is very mild, in its initial stages, simply refraining from swimming or washing hair for a few days, and keeping all implements out of the ear, usually results in resolution. External otitis is often a self-limiting condition. However, if the infection is moderate to severe, or if the climate is humid enough that the skin of the ear remains moist, spontaneous improvement may not occur.
Effective solutions for the ear canal include acidifying and drying agents, used either singly or in combination.[11] When the ear canal skin is inflamed from the acute otitis externa, the use of dilute acetic acid may be painful.
Burow's solution is a very effective remedy against both bacterial and fungal external otitis. This is a buffered mixture of aluminium sulfate and acetic acid, and is available without prescription in the United States.[12] But, Bayer does not officially recommend the use of the Burow's solution in the ear[13].
Topical solutions or suspensions in the form of ear drops are the mainstays of treatment for external otitis. Some contain antibiotics, either antibacterial or antifungal, and others are simply designed to mildly acidify the ear canal environment to discourage bacterial growth. Some prescription drops also contain anti-inflammatory steroids, which help to resolve swelling and itching. Although there is evidence that steroids are effective at reducing the length of treatment time required, fungal otitis externa (also called otomycosis) may be caused or aggravated by overly prolonged use of steroid-containing drops. In addition to topical antibiotics, oral anti-pseudomonal antibiotics can be used in case of severe soft tissue swelling extending into the face and neck and may hasten recovery.
Removal of debris (wax, shed skin, and pus) from the ear canal promotes direct contact of the prescribed medication with the infected skin and shortens recovery time. This is best accomplished using a binocular microscope. When canal swelling has progressed to the point where the ear canal is blocked, topical drops may not penetrate far enough into the ear canal to be effective. The physician may need to carefully insert a wick of cotton or other commercially available, pre-fashioned, absorbent material called an ear wick and then saturate that with the medication. The wick is kept saturated with medication until the canal opens enough that the drops will penetrate the canal without it. Removal of the wick does not require a health professional. Antibiotic ear drops should be dosed in a quantity that allows coating of most of the ear canal and used for no more than 4 to 7 days. The ear should be left open. Do note that it is imperative that there is visualization of an intact tympanic membrane (eardrum). Use of certain medications with a ruptured tympanic membrane can cause tinnitus, vertigo, dizziness and hearing loss in some cases.
Although the acute external otitis generally resolves in a few days with topical washes and antibiotics, complete return of hearing and cerumen gland function may take a few more days. Once healed completely, the ear canal is again self-cleaning. Until it recovers fully, it may be more prone to repeat infection from further physical or chemical insult.
Effective medications include ear drops containing antibiotics to fight infection, and corticosteroids to reduce itching and inflammation. In painful cases a topical solution of antibiotics such as aminoglycoside, polymyxin or fluoroquinolone is usually prescribed. Antifungal solutions are used in the case of fungal infections. External otitis is almost always predominantly bacterial or predominantly fungal, so that only one type of medication is necessary and indicated.
Prognosis
Otitis externa responds well to treatment, but complications may occur if it is not treated. Individuals with underlying diabetes or disorders of the immune system are more likely to develop complications, including malignant otitis externa. In these individuals, rapid examination by an otolaryngologist (ear, nose, and throat physician) is very important.
- Chronic otitis externa
- Spread of infection to other areas of the body
- Necrotizing external otitis
Necrotizing external otitis (malignant otitis externa)
This uncommon form of external otitis occurs mainly in elderly diabetics, being somewhat more likely and more severe when the diabetes is poorly controlled. Even less commonly, it can develop due to a severely compromised immune system. Beginning as infection of the external ear canal, there is extension of infection into the bony ear canal and the soft tissues deep to the bony canal. The hallmark of malignant otitis externa (MOE) is unrelenting pain that interferes with sleep and persists even after swelling of the external ear canal may have resolved with topical antibiotic treatment.
Natural history
MOE follows a more chronic course than ordinary acute otitis externa. There may be granulation involving the floor of the external ear canal, most often at the bony-cartilaginous junction. Paradoxically, the physical findings of MOE, at least in its early stages, are often much less dramatic than those of ordinary acute otitis externa. In later stages there can be soft tissue swelling around the ear, even in the absence of significant canal swelling. Also it can hurt the tip of your throat, causing pain when touched.
Treatment of MOE
Unlike ordinary otitis externa, MOE requires oral or intravenous antibiotics for cure. Diabetes control is also an essential part of treatment. When MOE goes unrecognized and untreated, the infection continues to smolder and over weeks or months can spread deeper into the head and involve the bones of the skull base, constituting skull base osteomyelitis (SBO). The infecting organism is almost always pseudomonas aeruginosa, but it can instead be fungal (aspergillus or mucor). MOE and SBO are not amenable to surgery, but exploratory surgery may facilitate culture of unusual organism(s) that are not responding to empirically used anti-pseudomonal antibiotics. The usual surgical finding is diffuse cellulitis without localized abscess formation. SBO can extend into the petrous apex of the temporal bone or more inferiorly into the opposite side of the skull base.
Complications
As the skull base is progressively involved, the adjacent exiting cranial nerves and their branches, especially the facial nerve and the vagus nerve, may be affected, resulting in facial paralysis and hoarseness, respectively. If both of the recurrent laryngeal nerves are paralyzed, shortness of breath may develop and necessitate tracheotomy. Profound deafness can occur, usually later in the disease course due to relative resistance of the inner ear structures. Gallium scans are sometimes used to document the extent of the infection but are not essential to disease management. Skull base osteomyelitis is a chronic disease that can require months of IV antibiotic treatment, tends to recur, and has a significant mortality rate.
See also
- Waterborne diseases
- List of cutaneous conditions
References
- ↑ 1.0 1.1 Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 1-4160-2999-0.
- ↑ Wang MC, Liu CY, Shiao AS, Wang T (August 2005). "Ear problems in swimmers". J Chin Med Assoc 68 (8): 347–52. doi:10.1016/S1726-4901(09)70174-1. PMID 16138712.
- ↑ http://www.ent.uci.edu/surfer%27s%20ear.htm
- ↑ Cobet AB, Wright DN, Warren PI (June 1970). "Tektite-I program: bacteriological aspects". Aerosp Med 41 (6): 611–6. PMID 4392833.
- ↑ Ahlén C, Mandal LH, Iversen OJ (July 1998). "Identification of infectious Pseudomonas aeruginosa strains in an occupational saturation diving environment". Occup Environ Med 55 (7): 480–4. doi:10.1136/oem.55.7.480. PMID 9816382.
- ↑ Thalmann, ED (1974). "A Prophylactic Program for the Prevention of Otitis Externa in Saturation Divers.". United States Navy Experimental Diving Unit Technical Report NEDU-RR-10-74. http://archive.rubicon-foundation.org/3372. Retrieved 2008-07-22.
- ↑ Zichichi L, Asta G, Noto G (April 2000). "Pseudomonas aeruginosa folliculitis after shower/bath exposure". Int. J. Dermatol. 39 (4): 270–3. doi:10.1046/j.1365-4362.2000.00931.x. PMID 10809975. http://www.blackwell-synergy.com/openurl?genre=article&sid=nlm:pubmed&issn=0011-9059&date=2000&volume=39&issue=4&spage=270. Retrieved 2008-07-22.
- ↑ Kang K, Stevens SR. Pathophysiology of atopic dermatitis. Clin Dermatol 2003;21:116–121.
- ↑ van Balen F, Smit W, Zuithoff N, Verheij T (2003). "Clinical efficacy of three common treatments in acute otitis externa in primary care: randomised controlled trial". BMJ 327 (7425): 1201–5. doi:10.1136/bmj.327.7425.1201. PMID 14630756.Full text
- ↑ Roland P, Stroman D (2002). "Microbiology of acute otitis externa". Laryngoscope 112 (7 Pt 1): 1166–77. doi:10.1097/00005537-200207000-00005. PMID 12169893.
- ↑ Doc Vikingo (March/April 2007). "Swimmers Ear – Additional Advice About A Pesky and Sometimes Painful Problem". Diver's Alert Network: Alert Diver Magazine. http://www.awoosh.com/DocVikingo/Preventing_Swimmers_Ear.htm. Retrieved 2008-07-22.
- ↑ Kashiwamura M. Chida E. Matsumura M. Nakamaru Y. Suda N. Terayama Y. Fukuda S. The efficacy of Burow's solution as an ear preparation for the treatment of chronic ear infections. [Clinical Trial. Journal Article] Otology & Neurotology. 25(1):9–13, 2004
- ↑ http://www.bayercare.com/Domeboro_faqs.cfm
External links
- Fluid in the Middle Ear: A Guide for Parents, The Institute for Good Medicine at the Pennsylvania Medical Society
- What to do if your child has swimmer's ear from Seattle Children's Hospital
- DRTBALU.com Otolaryngology online
|
|||||||||||||||||||||||||||||||||||||||